
Tackling Mental Health with Digital-First, Data-First Approach
By Maria Kordit, VP, Community Engagement, The Garage
The proliferation of healthcare technology and data availability has opened new avenues in mental health clinical oversight, patient engagement paths, and support tools. Studies from 2023 have shown that 21% of U.S. adults have experienced at least one mental health condition since the pandemic, of which 55% have not received any treatment. The highest prevalence of mental health conditions is among our nation's future generation, with 30.6% of conditions experienced by young adults ages 18 to 25.
There is a clear shift from population health management strictly focusing on physical health, and signals that the time has come for providers and healthcare organizations to take on responsibility for a broader range of mental health issues to succeed in a rapidly changing healthcare landscape. We at The Garage strongly believe we can overcome the division in the healthcare world that creates an unnecessary schism between clinical care and the mental/behavioral well-being of the patients our clients serve.
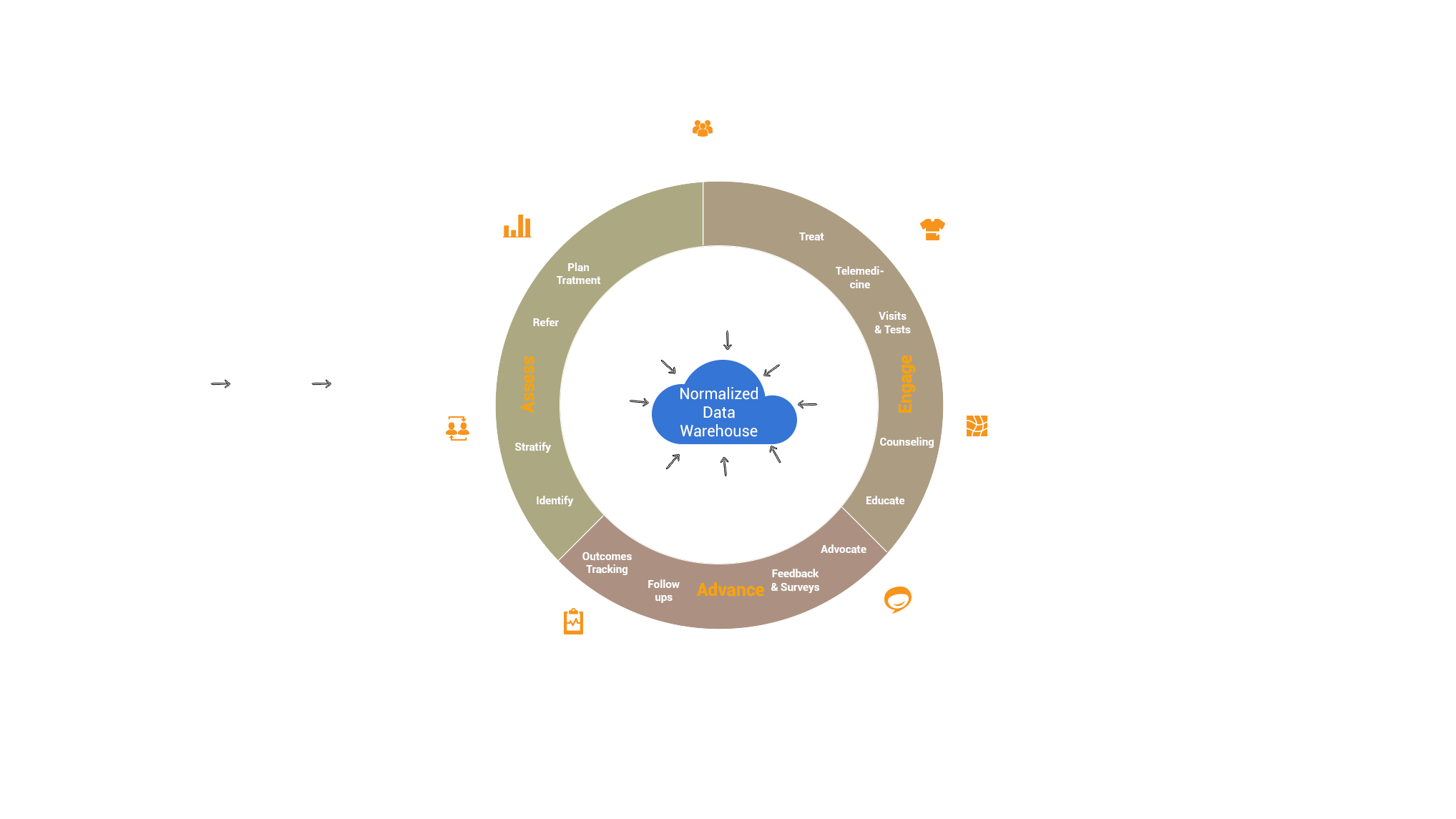
* This arch visual is proprietary to The Garage.
To achieve the adoption of mental health into the mainstream of patient care, there must be a unification of access via the digital-first strategy across all actors stemming from patients to care teams, partners, administrators, social support, researchers, family/friends, etc. through what we call the digital-front door. Behind the digital front door is the core of data being first and the driver of action and development. At the heart of this center core is a normalized data warehouse, where all various data sources feed into it, including but not limited to HIE data, pharmacy data, lab data, payer claims, EMR feeds, treatment facility data, patient-reported data, and financial details.
By focusing on being digital-first in access and data-first in solutions, we come to the second innermost layer that defines the patient's journey - assess, change, and advance. A patient will go through different experiences throughout these stages, which should be enabled via the front-door. To successfully empower such experiences for a patient's journey to sustainability, a set of solutions that are platform-based and offer unification of access to all should include care management, virtual care, patient engagement, care coordination, reports & analytics, and population management, all platform based.
Due to the nature and sensitivity of mental health in our nation, we must listen and respond to the needs of the patients we serve through listening, adjusting, measuring, engaging, interacting, connecting, personalizing, and analyzing all outcomes. This feedback loop is critical to assessing, realigning, and evaluating the impact on clinical outcomes.
All this ties together through blended and balanced systemic modalities that vary from Autonomous, In-Person, Asynchronous, and Synchronous touchpoints. This establishes a care continuum that is much needed for the growing mental health issues we face as a nation while simultaneously building a community model around individuals who often feel alone in their healing journey.
As population health management programs continue to grow and expand, we are excited to see new forging partnerships between healthcare providers and behavioral health/community services that help support the increasing pressure on primary care providers to help take on mental health support.
We believe this digital-first-data-first approach will not only unify data, users, and services in a way that allows for integrating mental health into mainstream healthcare but ultimately tackle the rising prevalence of untreated mental illness.
